Sean and Sharon had an idyllic first pregnancy. Their son, born in March 2016, was a healthy baby boy. Due to a family history concern, the couple had asked for genetic testing during this pregnancy. They ended up having sequential screening, which looks for chromosome conditions like Down syndrome that are not typically inherited. Their screening results were negative, so they “checked that box and just moved forward.” Given this unremarkable history, there was no reason for concern when they got pregnant with their second son in July 2018.
Sean and Sharon had an idyllic first pregnancy. Their son, born in March 2016, was a healthy baby boy. Due to a family history concern, the couple had asked for genetic testing during this pregnancy. They ended up having sequential screening, which looks for chromosome conditions like Down syndrome that are not typically inherited. Their screening results were negative, so they “checked that box and just moved forward.” Given this unremarkable history, there was no reason for concern when they got pregnant with their second son in July 2018.
What We Didn’t Know
Sharon was going to be nearly 35 years old when this second baby was born, so the couple was advised to do non-invasive prenatal testing (NIPT), a screening test with a higher detection rate and lower false-positive rate than sequential screening. Again, their NIPT was negative, and the tests showed they were having another boy. Sharon recalls “I remember being really excited that we were going to have two boys just three years apart.”
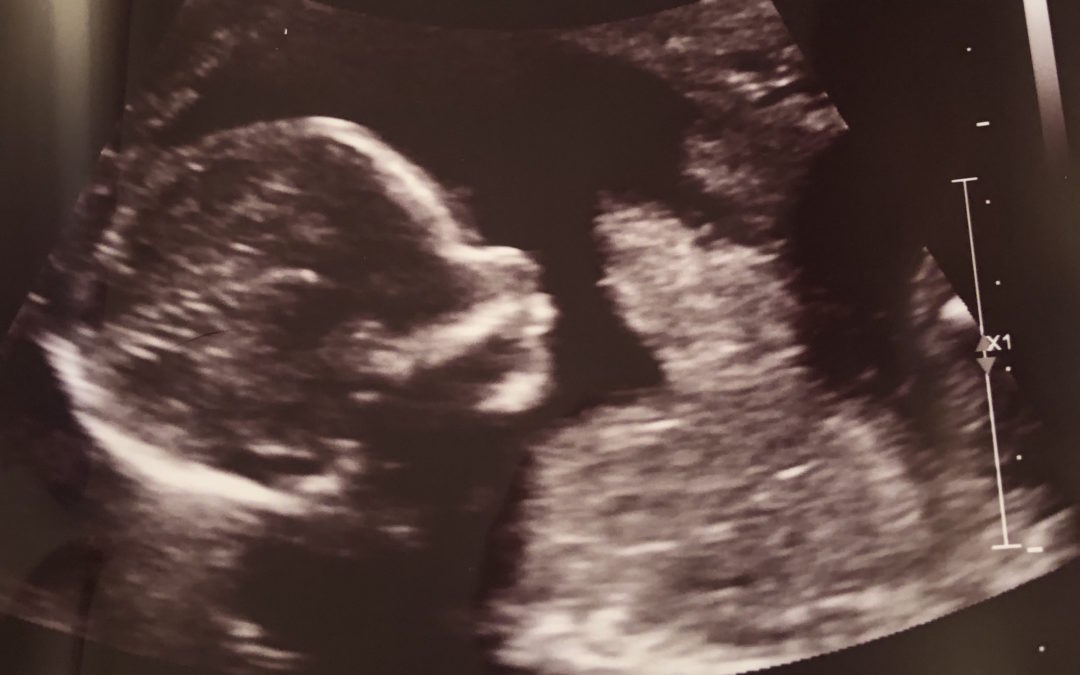
Not expecting any problems, Sharon went to her level II ultrasound by herself. The technician showed her the baby’s anatomy and printed out ultrasound pictures and then asked her to wait in a room for the doctor, who was in the process of delivering a baby. Sharon was a little confused, but still unconcerned. Until the doctor rushed in and said “We need to talk about these things we found on the ultrasound.” Sharon struggled to listen while trying to calm her mounting fear. The ultrasound had identified a single umbilical artery and an echogenic bowel. While neither were particularly problematic for the baby by themselves, they were “soft signs” that could be associated with chromosome conditions, bleeding, infection, or other genetic conditions like cystic fibrosis. Sharon was reassured that her NIPT results were negative, essentially ruling out the concern for chromosome conditions, and that echogenic bowel was “usually nothing.” She was tested for cytomegalovirus (CMV), the  infection most commonly associated with echogenic bowel, and a carrier screening panel was drawn to test for cystic fibrosis (CF).
infection most commonly associated with echogenic bowel, and a carrier screening panel was drawn to test for cystic fibrosis (CF).
Sharon’s CMV results were negative, but her carrier screening results were not. She was found to be a carrier for CF. Immediately, Sean’s blood was drawn and sent off for analysis. CF is an autosomal recessive condition, so both parents have to be carriers in order for a baby to be at risk for the condition. The result came back within days. It, too, was positive. An amniocentesis was performed the same day to find out if the baby had CF. Sharon says “That day that Sean’s test came back positive and we had the amnio. That was the worst day. It was when I finally felt shocked…and scared.”
The Waiting
While waiting for the results of the amnio, Sean and Sharon, both PhD scientists, started scrambling for information. Sean spent the next few days pouring over any and every piece of information he could find about CF, the range of prognoses, and their options. Their genetic counselor had given them the link to the Cystic Fibrosis Foundation, but Sean felt like it was mainly a resource for families whose children had been born with CF unknowingly. He and Sharon had a choice to make about whether or not they would continue this pregnancy, and to make that choice, they needed unbiased information about what CF could look like for their child. Both Sean and Sharon are carriers of classic CF mutations, meaning if the pregnancy was affected, their child would be expected to have a more severe case of CF.
The day after Thanksgiving, they finally received the results of the amnio. They were positive. Their son had CF.
Sharon remembers how incredibly sad that news was. Sean and Sharon had spent all that time while waiting for their amniocentesis results going through a decision tree, weighing pros and cons, analyzing their choices. They knew they needed to decide if they were going to continue the pregnancy or not because if they were going to terminate, they would have to move forward immediately. “We knew once we got the result, we wouldn’t have time to make any decisions, so we needed to already decide.” After reviewing all the information, looking at the mutations they had, and considering the potential impact of having a child with CF on their other young son, the couple decided to end the pregnancy. Sharon said, “I wonder if I would have felt differently if it was my first child. I don’t know. At the time, I had a 2.5 year old and all I could think about was every time he had been sick and that you just never want your kid to be sick at all.”
A New Path to Pregnancy
A few weeks after the termination, Sharon returned to her Maternal-Fetal Medicine (MFM) specialist for a follow-up appointment. This MFM had already mentioned the availability of preimplantation genetic testing (PGT) for CF on the day of her amnio, and at this visit, she reviewed all of their options for having another child, including IVF with PGT. Sean and Sharon knew they wanted another child and both felt strongly that they did not want to go through another termination. “For us, it felt kind of reckless. Before we didn’t know. Now we know, and we feel like we would not want to do this again on purpose.”
After doing some research, the couple found out that Sean’s company’s health insurance plan covers up to $40,000 towards IVF with an additional $20,000 in prescriptions. The desire to have something positive to focus on, the realization that cost would not be a barrier, and the understanding that the IVF with PGT process can take awhile led the couple to move forward quickly. They went to their first appointment with the fertility clinic in January of 2019.
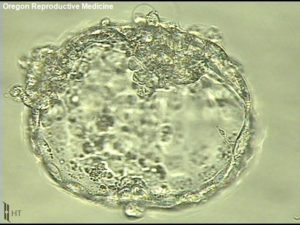 Sean and Sharon were lucky to have quick success with IVF. Their first IVF cycle yielded 10 viable embryos. Of those ten, 4 were trisomies, 2were mosaic, 2 were carriers of CF, 1 was affected with CF, and 1 was neither a carrier of CF nor affected with CF. That one embryo was transferred and the couple is currently pregnant with a CF-free baby girl! At this point, Sharon is anxiously awaiting the birth of her daughter. The worry of the past two years has taken a toll. She says “I just feel really focused on getting to the end and making sure everything is okay and just being thankful that she’s healthy.”
Sean and Sharon were lucky to have quick success with IVF. Their first IVF cycle yielded 10 viable embryos. Of those ten, 4 were trisomies, 2were mosaic, 2 were carriers of CF, 1 was affected with CF, and 1 was neither a carrier of CF nor affected with CF. That one embryo was transferred and the couple is currently pregnant with a CF-free baby girl! At this point, Sharon is anxiously awaiting the birth of her daughter. The worry of the past two years has taken a toll. She says “I just feel really focused on getting to the end and making sure everything is okay and just being thankful that she’s healthy.”
Take Home Lessons
Looking back on this entire journey, Sean and Sharon expressed three key takeaways.
- The importance of carrier screening. Sean and Sharon are PhD scientists. They are fascinated by numbers and statistics. Like, for example, that 1 in 25 Caucasian individuals is a carrier for cystic fibrosis. They remain surprised and frustrated that their health care providers never mentioned carrier screening to them or how important it can be, even in the absence of family history. Sean says, “In retrospect, that’s something we would have really taken seriously had the appropriate level of caution been provided to us.”
- The need for universal insurance coverage for fertility services. Sharon says, “Most people that I tell about it (IVF with PGT) are amazed that you can do that. People don’t know that PGT-anything exists. I feel really strongly that it should be covered by insurance. It’s a huge issue of equity…The whole process just made me feel very privileged to be able to do it.” While there are organizations working diligently to improve insurance coverage for fertility services, cost remains the primary barrier that prevents couples from pursuing IVF with PGT.
- The gift of sharing your story. When Sean went back to work after the termination, he just started telling people about his experience. The whole thing. In detail. While that may sound overwhelming, what he found is that it opened the door for other people to share their stories. Sharon says “We’ve really gotten to learn a lot of other people’s stories that we otherwise wouldn’t have known. That’s really special.”
We thank this family for sharing their story and look forward to congratulating them on the birth of that baby girl in May.
If you would like to learn more about IVF with PGT, please reach out to our genetic counseling team. It is our goal to make this technology accessible to every family who is at risk for a genetic condition.
.

Jessica Greenwood is an independent consultant to Sharing Health Genes. As a licensed genetic counselor and digital health consultant, she works with health-related organizations looking to deliver memorable messages of health in the digital space. Mrs. Greenwood started her career in a clinical role, working for eight years as a preconception and prenatal genetic counselor before transitioning to industry. Mrs. Greenwood completed a year-long certificate program in Digital Health Communication at Tufts University that spearheaded her work in digital health. She now consults with health-related organizations, assisting with the creation and execution of a digital strategy including the development of health literate patient-centered educational materials. Mrs. Greenwood earned a Bachelor of Science degree from North Carolina State University with a minor in Genetics and a Master of Science in Genetic Counseling from the University of North Carolina at Greensboro.